Mucormycosis, also known as 'Black Fungus', is a very rare infection. It is caused by exposure to mucor mold which is commonly found in soil, plants, manure, and decaying fruits and vegetables. According to doctors, it is universal and is found in soil, air, and even in the nose and mucus of healthy people. The condition does not spread from person to person and is not contagious.
The black fungus affects the sinuses, the brain, and the lungs and can be life-threatening in diabetic or severely immunocompromised individuals, such as cancer patients or people with HIV/AIDS. Reports of COVID-associated mucormycosis have generally been rare. A study of the medical literature traced eight cases reported around the world by 9 January 2021. In these reports, the most common risk factor for mucormycosis was diabetes. Early aggressive treatment is considered essential. It has been estimated that between 40% and 80% of people who contract any form of mucormycosis die from the disease, depending on the site of infection and underlying health conditions.
COVID-associated mucormycosis has especially affected people in India. One explanation for why the association has surfaced remarkably in India is high rates of COVID infection and high rates of diabetes. The black fungus also appeared in Russia. Due to its rapidly growing number of cases, the Rajasthan Government declared it an epidemic on 19 May 2021. Along with the Rajasthan government, the governments of Haryana, Tamil Nadu, Telangana, Gujarat, and Bihar have also now declared this an epidemic.
Doctors say they are surprised by the severity and the frequency of this black fungus in India during the second wave, compared to some cases during the first wave last year.
SYMPTOMS:
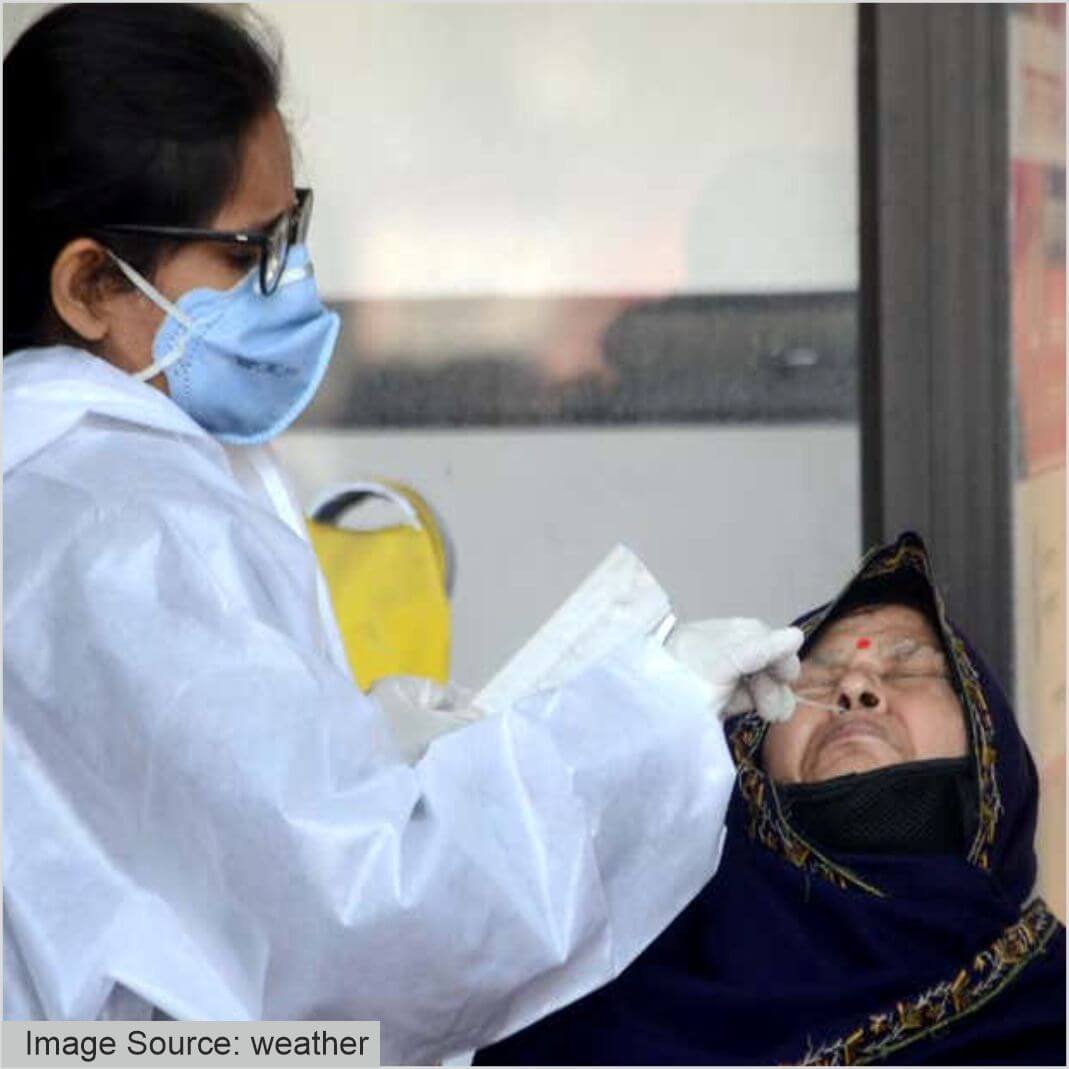
Black Fungus symptoms include pain and redness around the eyes or nose, fever, headache, coughing, shortness of breath, bloody vomits, and altered mental status. According to the advisory, infection with mucormycetes should be suspected when there is:
Black fungus infection carries a high mortality rate of 50%. However, if the disease is diagnosed in time, it can be treated well. According to doctors, the disease primarily infects the face, which is referred to as 'rhino-orbital-cerebral mucormycosis' and may even cause distinct facial deformities, associated with the disease.
TREATMENT:
Mucormycosis can prove to be quite dangerous if left untreated, and mutilate a patient's nose, jaw or alter the vital facial structure. The formation of black crusts, swelling in and around the nasal passage and the eyes is a peculiar feature. In many severe cases, surgeries may even be required to remove jaw bone or the nose.
While it is treated with antifungals, mucormycosis may eventually require surgery. Doctors have said that it is of utmost importance to control diabetes, reduce steroid use, and discontinue immunomodulating drugs. To maintain sufficient systemic hydration, the treatment includes an infusion of normal saline (IV) before infusion of amphotericin B and antifungal therapy, for at least 4-6 weeks.
Management of COVID patients with mucormycosis is a team effort involving microbiologists, internal medicine specialists, intensivist neurologists, ENT specialists, ophthalmologists, dentists, surgeons (maxillofacial/plastic), and others.
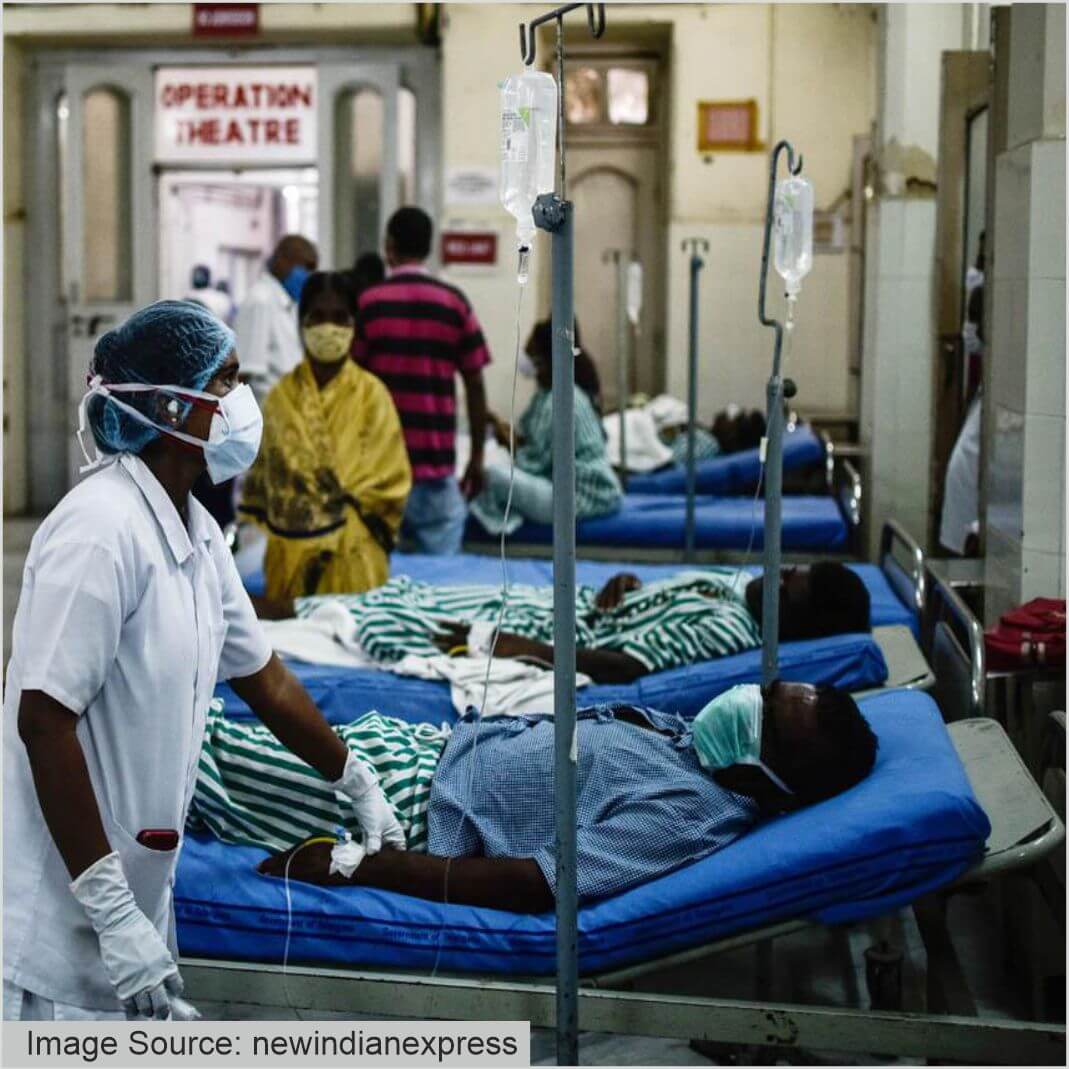
The disease is globally distributed, and generally pretty rare -- though it can be hard to place exact estimates of its prevalence due to lack of comprehensive surveillance and data.
The disease appears to be more common in India - one study by Indian microbiologists, published in March 2021, in the journal Microorganisms, suggested black fungus is 70 times more prevalent in India than in global data.
There are several possible reasons why -- there is a higher rate of "uncontrolled diabetes" in India, said the study. Many patients they studied didn't even know they had diabetes until they were diagnosed with black fungus, demonstrating "the lack of regular health check-ups in the Indian population," said the study.
Take utmost steps to ensure safety and hygiene. Keep your masks clean by washing cloth masks regularly and replacing surgical masks within an interval of 15-20 days. Get checked with your doctor as soon as you detect symptoms of COVID-19 and/or black fungus. It is essential for diabetic patients to follow all norms of safety to prevent getting affected by the epidemic.
